If you or a loved one has suddenly noticed weakness or paralysis on one side of the body after a stroke or injury, you’re not alone. Hemiplegia and Hemiparesis affect millions of Americans each year, mainly as a result of stroke, the leading cause of long-term disability in the United States.
These conditions can feel overwhelming, but understanding them is the first step toward recovery. This guide breaks down what they are, why they happen, and most importantly, how to manage them with the latest treatments and practical care strategies.
What Is Hemiplegia and Hemiparesis?
Hemiplegia and hemiparesis are neurological conditions that cause problems with movement on one side of the body. The prefix “hemi-” means “half,” so both involve only the left or right side.
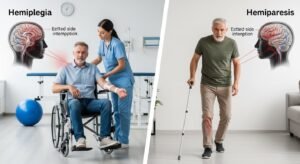
Hemiparesis refers to muscle weakness or partial loss of strength on one side. You might still move the affected arm or leg, but it feels heavy, clumsy, or hard to control.
Hemiplegia, on the other hand, means complete or near-complete paralysis, no voluntary movement at all on that side.
Both result from damage to the brain or spinal cord, and doctors often see them as points on the same spectrum rather than completely separate conditions. The severity depends on how many of the motor pathways are affected.
Key Difference Between Hemiplegia and Hemiparesis
The main difference is the degree of impairment. In hemiparesis, some muscle function remains; you may walk with a limp, lift your arm slowly, or grip objects weakly. In hemiplegia, the muscles on the affected side do not respond to commands at all, though sensation (feeling touch or pain) may still be present.
Think of it this way: hemiparesis is like trying to run with a heavy backpack on one shoulder, challenging but possible. Hemiplegia is like the backpack turning into a locked chain; movement stops completely. Early rehabilitation can sometimes shift hemiplegia toward hemiparesis as the brain rewires itself through neuroplasticity.
Causes of Hemiplegia and Hemiparesis
The most common cause in the U.S. is stroke. According to the CDC and American Heart Association data, nearly 800,000 Americans experience a stroke each year, and up to 80% of survivors develop motor deficits like hemiparesis or hemiplegia.
Other causes include:
- Traumatic brain injury (TBI) from falls, car accidents, or sports
- Spinal cord injury
- Brain tumors, infections, or bleeding
- Conditions such as multiple sclerosis, cerebral palsy (especially in children), or brain aneurysms
In children, perinatal or childhood stroke is a leading trigger, with about 60% of young survivors facing long-term hemiparesis or hemiplegia.
Symptoms of Hemiparesis
People with hemiparesis often describe:
- Weakness or heaviness in the arm, leg, or face on one side
- Difficulty with balance, walking, or fine motor tasks like buttoning a shirt
- Tingling, numbness, or “pins and needles” sensations
- Fatigue because the unaffected side works overtime
Daily activities like eating, dressing, or driving become frustrating but not impossible with therapy and adaptive tools.
Symptoms of Hemiplegia
Hemiplegia symptoms are more severe:
- Total inability to move the arm, leg, or both on one side
- Stiff or spastic muscles that may tighten involuntarily
- Drooping face or difficulty swallowing
- Complete loss of coordination on the affected side
Many people also experience shoulder pain (hemiplegic shoulder pain affects 24-64% of stroke patients) and need full assistance for transfers or mobility in the early stages.
Why Is Only One Side of the Body Affected?
Your brain controls the opposite side of your body because of a natural “crossover” called decussation. Nerve fibers cross over in the brainstem, so damage to the left side of the brain (which handles language and logic) typically causes right-sided hemiplegia or hemiparesis. Damage to the right side (which manages spatial awareness and emotions) often affects the left side.
This is why a left-brain stroke might bring speech problems alongside right-side weakness, while a right-brain stroke can cause left-side weakness plus neglect (ignoring the left side of space). Understanding this helps families anticipate additional challenges beyond movement.
Diagnosing Hemiplegia and Hemiparesis
Doctors diagnose these conditions through a combination of:
- Physical and neurological exams (testing strength, reflexes, and coordination)
- Brain imaging, such as MRI or CT scans, to locate the damage
- Sometimes, electromyography (EMG) or nerve conduction studies
Quick diagnosis is critical, especially after a stroke, because the first 48 hours can make a huge difference in recovery.
Complications of Hemiplegia and Hemiparesis
Beyond movement loss, complications include:
- Muscle spasticity and contractures (tightening that limits the range of motion)
- Chronic shoulder or joint pain
- Balance problems leading to falls
- Urinary incontinence or swallowing difficulties
- Emotional challenges: depression, anxiety, and “learned non-use” (avoiding the weak side) affect many patients and caregivers
Psychological support is just as important as physical therapy.
Treating Hemiplegia and Hemiparesis
Treatment starts with addressing the underlying cause (clot-busting drugs for stroke, surgery for tumors, etc.). Rehabilitation is the cornerstone:
- Physical and occupational therapy to rebuild strength and retrain the brain
- Constraint-induced movement therapy (forcing use of the weak side)
- Medications to reduce spasticity
Emerging options available in many U.S. centers (as of 2026) include:
- Robot-assisted therapy and virtual reality (VR) systems that make repetitive exercises engaging and precise
- Transcranial direct current stimulation (tDCS) paired with VR robotics to boost brain plasticity
- New electromagnetic network-targeted field (ENTF) therapy, shown in recent trials to reduce disability when combined with physical therapy
Early, intensive rehab, starting within days, gives the best outcomes.
Best Care for Hemiplegia and Hemiparesis
The best care combines medical treatment with daily-life strategies:
- Home modifications: grab bars, raised toilet seats, one-handed kitchen tools
- Assistive devices: braces, canes, or Saebo-style gloves for hand function
- Caregiver training and respite support to prevent burnout
- Mental health resources: counseling, support groups through the American Stroke Association or Children’s Hemiplegia & Stroke Association
- Long-term planning: school IEPs for kids, workplace accommodations, and aging-with-disability strategies
Consistency at home matters as much as clinic visits.
FAQs
What Is the Difference Between Hemiplegia and Hemiparesis?
Hemiparesis is weakness; hemiplegia is paralysis. Both affect one side, but hemiparesis allows some movement while hemiplegia does not. Many patients start with hemiplegia and improve toward hemiparesis with therapy.
Why Does Hemiplegia Occur?
It occurs when the brain or spinal cord’s motor pathways are damaged, most often by stroke, interrupting signals to one side of the body due to the natural crossover of nerves in the brainstem.
When Should You Seek Help for Hemiplegia or Hemiparesis?
Immediately. Sudden one-sided weakness or paralysis is a medical emergency; call 911. Even mild symptoms deserve prompt evaluation to prevent worsening and start rehabilitation early.
How Can Hemiplegia and Hemiparesis Be Treated?
Through targeted rehabilitation, medications, and emerging technologies like robotic VR and brain stimulation. Recovery is possible years later thanks to neuroplasticity.
Where Can You Find Support for Hemiplegia and Hemiparesis?
The American Stroke Association, local stroke clubs, online communities, and organizations like the Children’s Hemiplegia & Stroke Association offer resources, support groups, and caregiver programs across the U.S.
Conclusion
Hemiplegia and hemiparesis change life in an instant, but they do not define it. With today’s advanced rehabilitation, compassionate care teams, and strong support networks, most people regain meaningful independence and quality of life. If you’re facing this challenge, reach out to your neurologist or a certified stroke center right away. Knowledge, early action, and persistence are your strongest allies. You’ve got this, one step, one day at a time.
Share this guide with anyone who needs it, and remember: recovery stories are being written every day in clinics and living rooms across America.














